
Beth Ramsay’s lasting memory of her son’s surgery wasn’t the fear she experienced when he was taken from her arms for the procedure. It was that he giggled and smiled so soon after, despite his eyes being swollen shut and his head bandaged.
“Nick’s experience was definitely a lesson for me in how resilient kids are,” she says, reflecting on the skull surgery her son had as an infant and the specialized helmets he needed after. “He was a trooper throughout.”
A mom’s persistence
Nick’s years-long medical journey began at birth. “His head was pushed in on one side,” Beth explains, “and his left brow was pushing down over his eye, making it almost permanently closed. His right eye was significantly bigger, like it was pulled open.” Concerned, she asked doctors at the hospital about it, then his pediatrician, but couldn’t get anyone to take it seriously. “They just said to me: ‘People are asymmetrical.’”
Already a mom to a three-year-old, Beth’s experience told her it was something more. Researching on her own, she came across information about a condition that affects infant head shape called craniosynostosis. Right away, she realized she might be on to something.
A newborn baby’s skull is not yet a solid shape. It’s made of several bony plates connected by flexible material called sutures. In the first years of life, the brain grows rapidly and the sutures allow the skull to grow at the same rate.
Craniosynostosis occurs if one or more of the sutures fuse, or close, too early. This causes the bones to join together too early, which stops skull growth in those areas. The parts of the skull that aren’t fused will continue to expand as the brain grows, while the parts that are already fused together don’t, and this uneven growth can affect the shape of the head. Craniosynostosis can affect the appearance of the face also, as it did in Nick’s case. What causes it to occur is not exactly clear, but evidence shows it may relate to the baby’s position in the womb or to a child’s genes.
A big decision
Soon after learning about this, Beth connected with pediatric neurosurgeon Dr. Ann Ritter. “And I’m so glad I did,” she remarks. Dr. Ritter confirmed that Nick’s right coronal suture was closed. This is the suture that runs from the outside of the right eye to the soft spot at the top of a baby’s head. “It can be tough when kids don’t look like other kids. Dr. Ritter did a great job easing my fears, keeping everything in perspective and reassuring us that we really did have a healthy child.”
The more a child’s head shape becomes affected as they grow, the greater the worry about the effect on the brain, so timing matters when treating this condition. Surgery is typically recommended and generally performed before a child turns one. For children under six months, there are two options: minimally invasive endoscopic strip surgery, where the fused suture is removed through small incisions, and cranial vault remodeling, where the skull is surgically expanded to relieve pressure on the brain, create a normal head shape and allow for future growth.
Dr. Ritter worked with Beth and her husband to determine the best way to proceed for Nick’s needs and for their family. “She was the best,” Beth recalls. “Plain talk the entire time. Down to earth. Positive. We were faced with a lot of information, but never felt overwhelmed. This hasn’t been my experience anywhere else – you often get ‘doctor speak,’ but you don’t get that here. She even helped us find a second opinion.”
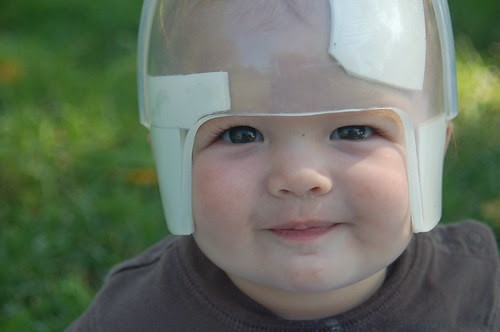 They chose endoscopic strip surgery and Nick had the procedure when he was about two months old. With this option, a child is required to wear a helmet that applies gentle pressure to mold the head as it continues to grow and for about a year following his surgery, Nick wore a helmet for 23 hours each day.
They chose endoscopic strip surgery and Nick had the procedure when he was about two months old. With this option, a child is required to wear a helmet that applies gentle pressure to mold the head as it continues to grow and for about a year following his surgery, Nick wore a helmet for 23 hours each day.
Numerous helmets were needed to keep up with his head growth and his parents decorated each new one with different stickers – bugs, race cars, etc. and often his name on the front. Beth worried at first that being in a helmet would cause Nick to miss some of his important “babyhood” moments, but he wasn’t slowed down. “He didn’t care at all,” she admits. “And the trade-off was worth it. We are so grateful for the outcome he’s had.”
Our craniofacial team monitored Nick in the years that followed. This team specializes in conditions that affect the face and skull and has experts from more than 15 different specialty areas who provide coordinated care as a child grows. What they watched for with Nick included facial asymmetry; vision, hearing and speech; and dental and orthodontic needs. He came for multidisciplinary clinic appointments at least once a year. “Having everyone in one spot on one day is really helpful,” Beth points out.
A distant memory
Now 11, Nick has no memory of his surgery or helmet, and he no longer sees the craniofacial team. “Visually he’s in a good place and experiencing no associated issues,” Beth reports thankfully.
About to finish fifth grade at Richmond’s William Fox Elementary School, his parents were recently told by a school staff member how kind and compassionate Nick is to his classmates, something they’re as proud to hear about as his strong academic focus. He’s quietly funny, into drawing comics and also loves sports. His active summer kicks off with a soccer tournament in early June. Swim meets begin soon after.
Looking back, when Beth recounts the challenging start to Nick’s life, the exact details of his treatment timeline are a fuzzy, distant memory. What she does remember with complete clarity though, is how her family and newborn son were treated throughout. “We received excellent care the whole time,” she emphasizes. “Very loving, individualized, compassionate, informative and down to earth. Always now, when I go into a hospital, I am so grateful that people do that work in the world.”
