
VCU researchers’ study of COVID-19 death rates and other variables is being shared worldwide and is guiding other studies, including an analysis from Goldman Sachs on face masks and GDP.
According to 198-country analysis, early face mask policies and guidelines curbed COVID-19’s spread.
Why have some countries, such as Italy and the United States, faced major public health crises with COVID-19 cases and related deaths, while others seem to have watched the pandemic come and go as merely a blip on the radar?
A new study led by Virginia Commonwealth University’s Christopher Leffler, M.D., currently in the peer review process, indicates that when governmental face mask requirements were put in place is a big factor.
Leffler, an ophthalmologist at VCU Health and Children’s Hospital of Richmond at VCU, and the other study authors looked at multiple variables across 198 countries, including age, sex ratio, obesity prevalence, temperature, urbanization, smoking, duration of infection, lockdowns, viral testing, contact tracing policies and mask wearing norms and policies.
The study found that the single most important factor that can be controlled is wearing masks in public.
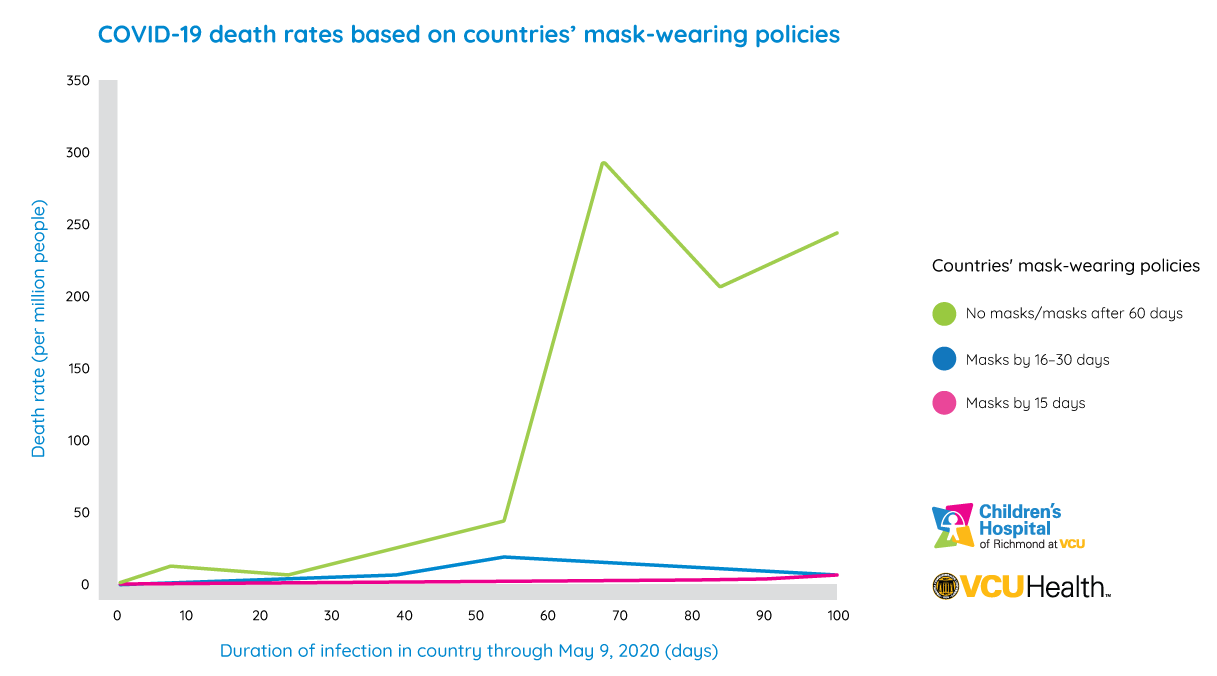
“In countries that recommended face masks early on a national level, or those in which the public wore them early based on cultural norms, the COVID-19 death rate has been lower than projected,” said Leffler, an associate professor in the Department of Ophthalmology at the VCU School of Medicine. “And it’s not just by a few percent, but up to a hundred times lower mortality.”
 Initial recommendations in the U.S. were that face masks should be reserved for health care workers and only worn by members of the general public who were experiencing symptoms. The Centers for Disease Control and Prevention then recommended that all Americans wear masks in public beginning April 3, a couple of weeks after all 50 states had reported cases of COVID-19. Meanwhile, several countries in Asia, including Thailand, Japan, Taiwan and Hong Kong, which maintains a separate governing system from that of mainland China, began using masks very early and have since demonstrated their effectiveness.
Initial recommendations in the U.S. were that face masks should be reserved for health care workers and only worn by members of the general public who were experiencing symptoms. The Centers for Disease Control and Prevention then recommended that all Americans wear masks in public beginning April 3, a couple of weeks after all 50 states had reported cases of COVID-19. Meanwhile, several countries in Asia, including Thailand, Japan, Taiwan and Hong Kong, which maintains a separate governing system from that of mainland China, began using masks very early and have since demonstrated their effectiveness.
“A number of countries in Asia still have mortality close to 1 in 1 million or less. In the U.S. right now, our coronavirus mortality is 1 in 2,500 people in the population,” added Leffler.
Italy, Spain, France and the United Kingdom also implemented mask-wearing policies much later and have had similarly high rates of infection and death. This is critical information as states, including Virginia, begin the next phase of reopening with looser restrictions on gathering and entering public spaces — and as health officials warn that another wave of COVID-19 is possible.
“It's very important for people to wear masks when we’re around others, particularly when indoors. That's the bottom line,” Leffler said. “This study shows it really can make a difference in preventing the spread of infection and helping us do all the things we want. We want kids to be back in school. We want businesses to be open. We want to live our normal lives.”
Masks do not need to be medical quality or prohibitively expensive. When worn properly over the nose and mouth, store-bought or homemade cloth masks can be effective in preventing the spread of respiratory droplets and coronavirus.
It’s key to continue frequent and thorough hand-washing, along with social distancing to limit the spread of coronavirus as well.
Leffler brings a unique background and perspective to the study, having completed a residency in occupational and environmental medicine. He also earned a master’s degree in public health and served as an undersea medical officer in the Navy. The study, which has been widely shared by researchers, was the most-read paper by a U.S. author during the week of June 22 on the international research database ResearchGate.
“This study from Dr. Leffler and our School of Medicine team underscores the science behind how important it is to wear a mask to prevent the spread of COVID-19,” said Peter Buckley, M.D., interim CEO of VCU Health System and interim senior vice president of VCU Health Sciences. “As the CDC has stated — and as this study’s data shows — cloth face masks are most effective when used widely in public settings.”
Leffler, the study’s lead author, collaborated with co-authors from VCU, Central Virginia VA Health Care System, the University of Toronto, the University of Miami, the University of Warmia and Mazury in Olsztyn, and the Poland Institute for Research in Ophthalmology.
Two additional factors when controlling for other variables were the age of the population, specifically those over 60, and urbanization, Leffler and his co-authors found. These results were not surprising, given that older adults tend to have more adverse outcomes with infection when compared to people who are younger. Cities, where social distancing is often more difficult, are also being hit harder in terms of infection and per capita coronavirus-related mortality rates.
Other factors, such as smoking rate and household income, did not appear to be as significant in affecting mortality due to COVID-19, while less-controllable environmental factors, such as temperature, humidity and sunlight, may be relevant and warrant further investigation.
This research continues to guide studies on related topics, including a Goldman Sachs analysis on the role of face masks in the spread of coronavirus and the associated impact on gross domestic product.
The global investment firm confirmed Leffler’s findings and proposed that a national face mask mandate could theoretically substitute for stay-at-home orders and improve GDP.


.jpg)