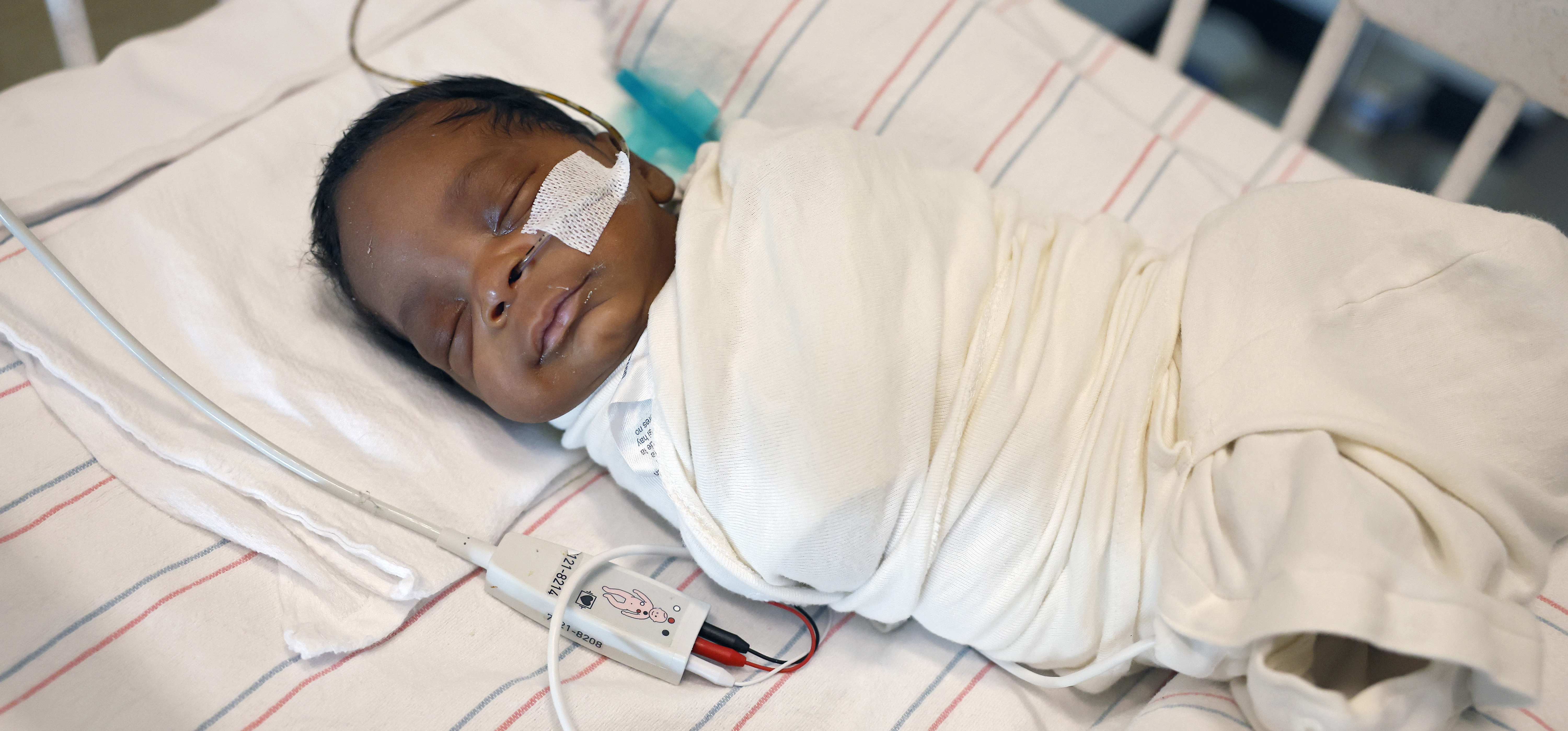
Mother nature, unsafe conditions and treacherous travel didn’t stop teams at CHoR and VCU Health Community Memorial Hospital in South Hill from making sure a premature baby got the expert care he needed.
Danielle Hayes was 30 weeks pregnant with her third child and preparing to be admitted to the hospital in just a few days. She knew she needed to be closely monitored after being diagnosed with a serious and potentially life-threatening pregnancy complication called placenta previa. The condition happens when the placenta covers the cervix, blocking the baby’s exit and can cause severe bleeding, which can be fatal for both mom and baby.
Danielle did not want to take any chances. She lost her older sister in 2017 following complications from pre-eclampsia shortly after childbirth. Danielle’s sister died when her son was only three days old.
Doctors told Danielle she would be admitted at 31 weeks gestation because of her placenta previa, but in the days leading up to that, she was at home and discovered she was bleeding. She knew she had to get to the hospital as soon as possible and prepare for an emergency c-section. The date? It was January 25, the day Virginia was expecting dangerous amounts of snow and ice from the winter storm that had paralyzed much of the country, and the conditions outside were deteriorating.
Danielle made it to the hospital closest to her home in southside Virginia, VCU Health Community Memorial Hospital, but it doesn’t have a NICU and the weather was only getting worse.
“It was very, very bad. It was snowing,” said Danielle. “They were making preparations for an emergency c-section, but they did tell me that because of the weather, they couldn’t transfer us.”
While Community Memorial Hospital has a labor and delivery department, they typically deliver healthy or full-term babies and are only equipped to provide basic care. For sick newborns, they stabilize those tiny patients and prepare them to be transferred to the Level IV NICU at CHoR.
“I received a call around 9 a.m. from one of our transport nurses saying there was a pre-term baby being born at 30 weeks at CMH,” remembered Dr. Joseph Khoury, our interim chief of neonatal medicine and medical director of our neonatal-pediatric transport program. “They wanted us to be there for the delivery and bring the baby back to our NICU because they don’t have the capacity, expertise or equipment to take care of baby at that age.”
Normally, the transport team rushes into a helicopter or ambulance to get to our partner hospital, but that day, neither of those were options. All helicopters were grounded and because of all the ice and poor visibility, putting an ambulance on the road would be a big risk.
“We are always ready to help them in any way possible,” explained Dr. Khoury. “We wanted to be there for the baby and the mom, but we also always want to make sure we are considering the team’s safety at the same time.”
Although CHoR’s transport team couldn’t get to CMH, they still wanted to be there for that team and give them all the resources and support they could as they waited for weather conditions to improve. After multiple conversations a plan to safely deliver care was born-- and so was little Kamyrn Coleman. He entered the world 10 weeks early at 10:51 a.m. on January 25, weighing 3 pounds 9 ounces.
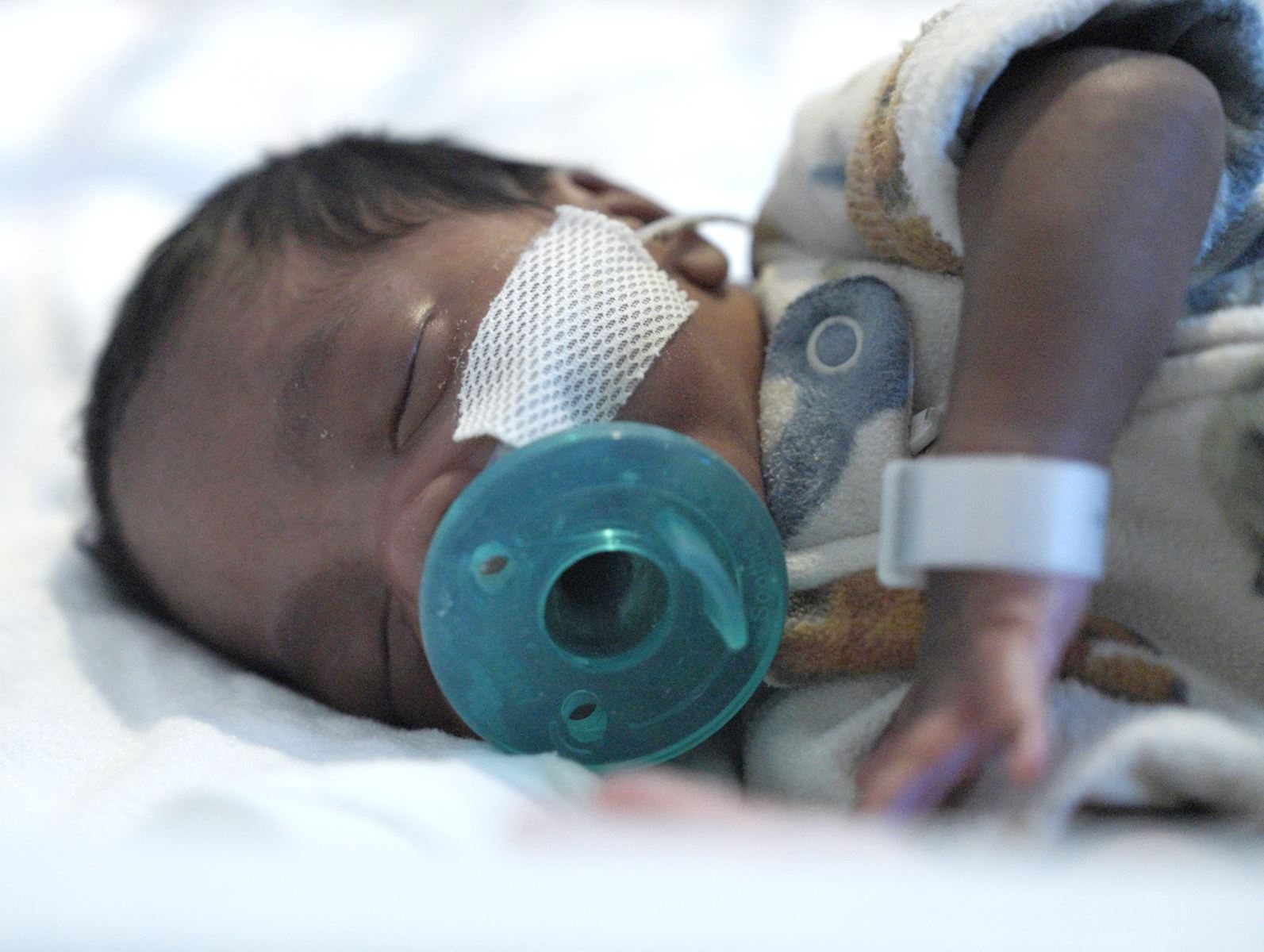
Taking care of a premature newborn remotely
“We knew that a baby at 30 weeks can have a lot of complications,” explained Dr. Khoury. “The outcome could have been very bad had we not been able to be there for the team.”
The solution? An ongoing virtual meeting on a tablet with the team at CMH and the transport nurse who would have been in the ambulance if it had been safe enough to travel, along with the attending neonatologist on duty, Dr. Mark Astoria. At the same time, CHoR leadership and the NICU doctors and nurses still worked diligently to get the team at CMH in-person help.
“With video conferencing, we can visually look at the baby and do some physical exams from visual assessments,” explained Dr. Astoria. “We can talk to the care team, give them some different guidance on different things to do or medical interventions. There’s also equipment that they’re not familiar with like the incubator and the ventilator and we can walk them through how to use them.”
Transport nurse Amy Potter spent her entire NICU shift monitoring Kamyrn’s progress, vitals, x-rays and labs remotely and providing support to the CMH team.
“I’m proud to work for a hospital that thinks outside the box,” said Amy. “We were able to come up with a plan to offer them a virtual care solution. I was given the opportunity to spend the day hanging out with them, even though I was here and they were there, and we basically took care of the baby together.”
While the CHoR NICU had a constant connection with the CMH team, CHoR president Elias Neujahr stayed in frequent contact with CMH president Sheldon Barr, which provided another, much appreciated, layer of support.
“Just being able to have that connection with Elias when all of this was going on, and him being calm allowed me to present a calm demeanor to my team, and that was invaluable,” explained Barr.
“This is what we do and why we are here,” explained Neujahr. “CHoR is committed to taking care of this community and all the patients who need us, and we strive to support our team in any way possible, no matter what obstacles we encounter.”
Shortly after Kamyrn was born, Dr. Astoria and Amy were relieved to see that initially the baby was doing well, but they know things can change in an instant and that a preemie’s condition can evolve throughout the day. Like Dr. Khoury and the leadership team, they really wanted to get CMH in-person help.
Providing support to CMH until it’s safe for the transport team
One of our NICU’s nurse practitioners, Monica Brakefield, actually lives in South Hill just 15 minutes away from CMH, but she was already on shift at CHoR. She had spent the night at the hospital so she didn’t have to drive in snow and ice.
She was on rounds that morning when she heard what was happening not far from her house. When Dr. Khoury approached her later in the day about lending her expertise to the CMH team in an area she knew very well, she didn’t hesitate to help.
Despite working almost her entire shift and sleeping at CHoR the night prior, Monica prepared to brave the elements and head south to support the CMH team and help take care of little Kamyrn.
Before she hit the road, she called her dad for guidance, who studied the radar.
“All dads act like they’re meteorologists and I asked him if it’s going to get worse,” explained Monica. “He said, ‘you actually have the perfect break, there’s nothing falling.’ Not only that, I was behind a snow plow the whole time and ice didn’t start falling again until I pulled into the parking lot at CMH. I was like, ‘Ok. This is a God thing. It has to be, there’s no other explanation.’”
Despite the break in the weather, a trip that would normally take 1 hour and 20 minutes took Monica 2 hours. While Monica was driving, Kamyrn started having to work harder to breathe. The CMH team, with instructions and support from Amy and Dr. Astoria, were able to intubate and stabilize their tiny patient.
Intubating an extremely premature baby isn’t something the CMH team normally does, but Dr. Khoury credits CHoR’s NICU outreach training for that success. The Outreach Program, led by Dr. Khoury and working closely with Dr. Jenny Fox, medical director of simulation, coordinates training at smaller hospitals, free-standing emergency departments and with EMS crews so teams can learn how to resuscitate and stabilize babies until our transport nurses can get there.
“It’s a huge win for them to be able to handle not only the intubation, but also the umbilical line that was needed,” explained Dr. Astoria. “This is something they don’t have to do on a regular basis, and to be able to utilize those skills and use them with a pre-term baby, while staying cool and calm, is remarkable.”
The CMH team was able to provide the life-saving measures Kamyrn needed in those crucial moments, but they were still very relieved when Monica arrived.
“I walked in and you could see everyone just exhale,” remembered Monica. “I was glad I was able to give them that breath, but they did great, they did all the hard work. They went above and beyond what they're trained to do. It could not have gone any smoother than it did.”
From that point on, Monica monitored Kamyrn’s progress, checked in regularly with the team at CHoR and made it clear she wasn’t going anywhere until it was safe for the newborn to be transferred.
Their first NICU graduation
The precipitation eased up overnight, and while Monica was able to sleep for a few hours at CMH, the decision was made that it was safe to dispatch a team to CMH to transport Kamyrn via ambulance to Richmond and CHoR’s NICU the following morning.
Even though CMH doesn’t have a NICU, they still wanted to give the type of sendoff NICU graduates get after they’re discharged from the hospital..png)
“We do a clap out. We have pompoms, we cheer, we play the graduation song, and they wanted to do that for Kamyrn because he was their first NICU baby,” explained Monica. “So, when our transport team arrived, one of the nurses comes in and says, ‘just so you know, this is going to be bigger than you think.’”
That nurse wasn’t exaggerating.
“We walked out and everybody’s cheering,” remembered Monica. “We got off the unit and it continued, there were people everywhere. When we got on the elevator, we were like, ‘that was great!’ But then we get off the elevator and there are even more people. I swear every employee in the hospital was lined up and all of them were excited and cheering.” Click here to watch the video!
Kamyrn’s unique entrance into the world was a first for Dr. Khoury as well.
“I’ve been here close to 13 years now and this is the first time we’ve ever experienced something like this,” Dr. Khoury recalled. “This event underscores the exceptional clinical skill, professionalism and dedication of our teams across institutions. I am deeply grateful to be part of such an exceptional NICU team and leadership community.”
Baby Kamyrn today
The baby that had the VCU Health community rallying around him in two parts of the state is continuing to grow and thrive. More than 7 weeks after his arrival, yet still 3 weeks ahead of his due date, he is preparing to be discharged from the CHoR NICU. He continues to reach milestones necessary for his release and his parents and his two older siblings can’t wait for him to come home. In the meantime, they know that the care he is receiving at CHoR will ensure he is ready to take on the world outside the hospital and they are so grateful.
“I just want to say thank you. Thank you to everyone, for all the prayers and for everything,” said mom. “I was so scared, but now he’s growing and doing so well.”

