Humanitarian outreach
Outreach
Members of our team donate their time and talents providing surgery and supportive services for children and families who do not have access to craniofacial care in their home countries. Below are some highlights of our outreach programming.

Providing speech therapy and feeding management in Honduras—2019 Mission Update
2019 marks Ruth Trivelpiece's ninth year providing speech and feeding services for World Pediatric Project in Honduras. Learn more about these efforts

Drs. Jennifer Rhodes and Gary Tye help Sophia fulfill her dream of returning home to Honduras — and just in time for school.
Learn more about Sofia

Formally conjoined twins adjusting well to separation
Children's Hospital of Richmond at VCU discharges twins Maria and Teresa Tapia after successful surgery. Read their story

A young life transformed before our very eyes
Just months ago, 10-year-old Oswaldo walked with his head down and was too embarrassed to make eye contact. Today he is thriving. Meet Oswaldo and learn about his surgery
Hope and healing for Baby Joel
When baby Joel was born, his mother Loralie immediately knew something was wrong. Learn more about Joel's surgery
Honduras 2019 Mission—Update
by Ruth Trivelpiece, speech-language pathologist and program coordinator, Center for Craniofacial Care (pictured)
2019 marked my ninth year providing speech and feeding services for World Pediatric Project in Honduras.
This year our team leaders from World Pediatric Project (WPP) and I traveled a day ahead of the surgical team to get a “head start.” We all needed extra time to make sure we could do the best job possible!
Speech therapy

I was able to evaluate many patients on Saturday before the team arrived at the Clinica Asturias medical facility and complete the thorough speech assessments needed to assist the surgeons with surgical planning. Children who have undergone cleft palate repair require very careful evaluation to determine if the palate is working properly for normal speech production. This can be a bit time consuming, especially when it needs to be done in Spanish! It is critical since the evaluation tells us if a child needs more surgery on the palate, needs to have a hole in the palate repaired, or has speech problems which need speech therapy and not surgery.
During the following week I had a full schedule of children coming in for speech therapy. Many children were seen in previous years and I was able to continue the therapy and work closely with the families. It was very rewarding to see them bring back their speech notebooks and flash cards. I made sure to save the last 15 minutes of every speech session to give the parents a chance to practice their skills as speech therapists. This year I used video so that I could review their sessions with their children and point out areas they were excelling in and techniques that needed extra practice. It was a great success and everyone loved seeing themselves on video!
Feeding
During the week I evaluated newborns with cleft lip and palate who were having difficulty with feeding. My heart went out to these families who were struggling to feed their babies. I am happy to report that all infants were sent home feeding successfully. All parents were able to use the special feeding bottles and were provided with enough bottles and nipples to last them until we return next year.
I supplied the Clinica Asturias with a feeding video produced by ACPA Family Services in case their nurses needed a “refresher” during the year. It was especially exciting because the video was recently translated into Spanish!
Each year I continue to learn what families need and how I can improve my service to them. I know to bring lots of toys and books to reward these hard-working children, and sets of articulation cards in Spanish for families to practice during the year. Parents in Honduras are just like parents here —everyone wants to see their children do their best. I am looking forward to seeing all “my” kids and families next year and meeting new families!
Hasta luego!
Sofia goes to school
 For most toddlers, using a crayon to scribble across a coloring page is a fun and easy task. But for 3-year-old Sofia, those precious scribbles are the product of three months of procedures, two surgeries and dedicated physical therapy.
For most toddlers, using a crayon to scribble across a coloring page is a fun and easy task. But for 3-year-old Sofia, those precious scribbles are the product of three months of procedures, two surgeries and dedicated physical therapy.
Sofia was born in Honduras with a rare condition called Apert syndrome. This condition left her with physical deformities in her fingers and toes as well as craniofacial deformities that put severe pressure on her brain. Without proper treatment, these deformities impact cognitive development and may cause blindness or be fatal. As a result, Sofia was unable to feed, dress or learn to care for herself. But Sofia's mother, Angela, refused to lose sight of her dream for Sofia, including her chance to attend school one day.
World Pediatric Project partners first met little Sofia during a mission to Honduras. During this trip, Dr. Gary Tye, chief pediatric neurosurgeon, recommended that Sofia travel to Richmond for live-saving surgery including facial reconstruction in order for her to grow and thrive like a normal toddler.
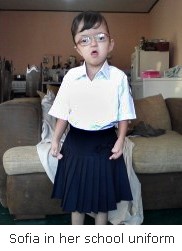 Several months later Dr. Tye and Dr. Jennifer Rhodes, director of our Center for Craniofacial Care, completed the required surgical procedures and Sofia was able to go home. Soon after getting back to Honduras, Sofia was able to hold a cup, and then a crayon, and even began helping her mother to dress her. Today, Sofia is not only coloring, but also fulfilling her lifelong dream of attending school.
Several months later Dr. Tye and Dr. Jennifer Rhodes, director of our Center for Craniofacial Care, completed the required surgical procedures and Sofia was able to go home. Soon after getting back to Honduras, Sofia was able to hold a cup, and then a crayon, and even began helping her mother to dress her. Today, Sofia is not only coloring, but also fulfilling her lifelong dream of attending school.
Brava Sofia!
Article provided by World Pediatric Project. To see more photos of Sofia please visit www.worldpediatricproject.org.
A young life transformed before our eyes
 Just months ago, 10-year-old Oswaldo walked with his head down and was too embarrassed to make eye contact, even with his family. Today he is thriving in school, making friends, and proudly showing his face to all.
Just months ago, 10-year-old Oswaldo walked with his head down and was too embarrassed to make eye contact, even with his family. Today he is thriving in school, making friends, and proudly showing his face to all.
Through the generosity of so many who support World Pediatric Project, Oswaldo is one of more than 2,000 children who received surgical or diagnostic care this past year. For Oswaldo and his family, it represented a miracle come true, and the fulfillment of a long and challenging journey for care.
Oswaldo was bore in a rural, Mayan region of Guatemala where his mother, like most of the rural population of the country, does not typically consume food rich in folate. This folate deficiency is linked to many congenital conditions such as spina bifida, cleft lip and cleft palate, and the condition Oswaldo was born with, which is called a nasal encephalocele. A nasal encephalocele is most often characterized by an opening in the skull near the forehead and nose from which brain matter protrudes. For Oswaldo, this condition was progressively worsening causing frequent severe headaches and vision trouble. The social stigma of his deformity also prevented him from attending school.
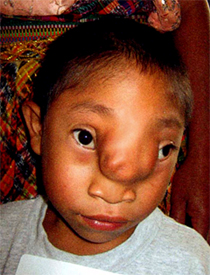 For years, Oswaldo's family sought help to repair Oswaldo's birth defect and was continually told help didn't exist in Guatemala. It wasn't until World Pediatric Project sent a pediatric neurosurgery team to the region that they finally had a home for him.
For years, Oswaldo's family sought help to repair Oswaldo's birth defect and was continually told help didn't exist in Guatemala. It wasn't until World Pediatric Project sent a pediatric neurosurgery team to the region that they finally had a home for him.
Although Dr. John Ward, pediatric neurosurgeon at Children's Hospital of Richmond at VCU, had travelled to Guatemala for more than 10 years, a recent World Pediatric Project surgery mission took him to a different region where he first met Oswaldo. Dr. Ward evaluated him and immediately recommended he travel to the U.S. for this complex surgery.
Plans to help Oswaldo moved forward quickly. Thanks to the combined volunteer efforts of Dr. Gary Tye, pediatric neurosurgeon at Children's Hospital of Richmond at VCU, and Dr. Jennifer Rhodes, pediatric plastic surgeon and director of the Center for Craniofacial Care at Children's Hospital of Richmond at VCU, Oswaldo's condition was successfully corrected through a 10-hour complex procedure. Oswaldo demonstrated his recovery in the most remarkable of ways - by reading one book after another!
 His brother Fernando remarks, “Oswaldo is so smart but couldn't attend school for fear of being teased.” Instead to pass the time and continue to learn, he read as much as he could until severe headaches overcame him.
His brother Fernando remarks, “Oswaldo is so smart but couldn't attend school for fear of being teased.” Instead to pass the time and continue to learn, he read as much as he could until severe headaches overcame him.
Today Oswaldo thrives. His brother recently revealed Oswaldo is not only in school for the first time in his life - but is rapidly becoming the best student in class! Because he loves to read and learn, he now hopes to become a teacher when he grows up.
Article provided by World Pediatric Project.
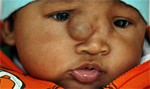
Hope and healing for Baby Joel
When baby Joel was born, his mother Loralie immediately knew something was wrong. Joel had been born with an abnormal growth on his face called an encephalocele, which threatened to end Joel's life.
Treatment of an encephalocele requires a complicated and potentially dangerous surgery to remove the growth and reconstruct the face. This surgery could not be done safely in the Belizean hospital. The medical resources and expertise simply were not available. But the defect continued to grow rapidly, placing Joel's life at risk. You could sense the fear she had that her baby would die if she could not find help for him.
 Joel and his mother were living in a 12-by-12-foot room with his aunt and 4-year-old cousin. All they had were two small beds and a small stove. They bathed outside using an outhouse for their toilet. Loralie earned 25 dollars a week washing her sister's and neighbors' clothes.
Joel and his mother were living in a 12-by-12-foot room with his aunt and 4-year-old cousin. All they had were two small beds and a small stove. They bathed outside using an outhouse for their toilet. Loralie earned 25 dollars a week washing her sister's and neighbors' clothes.
In November, James Pitre, the founder of Compassionate Hearts Alliance, was introduced to baby Joel and his mother while he was on a trip to Belize. James and his wife Lorrie are committed to assisting children with extreme medical conditions.
James contacted 13 university and children's hospitals before reaching out to the World Pediatric Project (WPP). This nonprofit organization based in Richmond, Virginia links pediatric surgical care to developing countries in Latin America and the Caribbean. IHC then contacted Children's Hospital of Richmond at VCU and its Center for Craniofacial Care.
 Pediatric craniofacial surgeon Dr. Jennifer Rhodes and pediatric neurosurgeon Dr. Gary Tye rapidly developed a treatment plan for baby Joel and agreed to donate their time to provide him with the care he needed. VCU Medical Center generously agreed to cover the cost of Joel's hospital stay. Since 2001, IHC and CHoR have worked together to provide over 150 children with complex medical conditions with free hospital care otherwise unavailable in their home countries.
Pediatric craniofacial surgeon Dr. Jennifer Rhodes and pediatric neurosurgeon Dr. Gary Tye rapidly developed a treatment plan for baby Joel and agreed to donate their time to provide him with the care he needed. VCU Medical Center generously agreed to cover the cost of Joel's hospital stay. Since 2001, IHC and CHoR have worked together to provide over 150 children with complex medical conditions with free hospital care otherwise unavailable in their home countries.
Joel and his mother arrived in Richmond on October 28, 2009, five days after IHC was initially presented with his case. Joel's surgery took place one week later.
Donating their services, Drs. Rhodes and Tye kept a close watch over Joel during his recovery from the lengthy and complicated surgery. After four weeks, Joel was ready to return to his home in Belize.
Joel's mother summed up their experience saying, “It seemed impossible. But now, Joel will grow up and have a future. Forever, we are grateful to you both and your entire staff at the VCU Medical Center.”
